interestingengineering.com
In a First, Genetically Modified Pig Heart Transplanted Into a Human
Xeno - cross-species transplants were impossible a few decades ago. Now science makes it possible and could help save thousands of lives in the future.
Science & Tech
Over six weeks ago, 57-year-old, David Bennet was admitted at the University of Maryland Medical Center (UMMC) with life-threatening arrhythmia - a condition where the heart beats irregularly.
His condition required him to be put on a heart-lung bypass machine and he would have to join the list of 110,000 Americans that are currently awaiting a donor organ for their transplant. But a heart from a genetically modified pig was used instead, making him the first human to receive one, a press release from the UMMC said.
Xenotransplantation - using an organ from a different species - was first attempted in the 1980s. An infant with a fatal heart condition received a transplant from a baboon but the transplanted organ was rejected by the infant's immune system resulting in her death a month after the procedure. Researchers have had much more success with pigs as donors, especially in the case of heart valves that have been used to replace faulty ones in humans, the press release said.
Virginia-based Revivicor has been experimenting with genetically modified pigs so that their bodies do not produce a sugar called, alpha galactose - which since is not produced by the human body is a telltale sign of a foreign body for the immune system. In October last year, the company trialed kidneys from such genetically modified pig on a dead human being to verify if it could be used as a transplanted organ. The company collaborated with the University of Maryland to develop compatible hearts.
According to the press release, the transplanted heart came from pigs that carried ten modified genes to improve compatibility with the human immune system. First three genes that trigger antibody-mediated rejection from the human immune system were removed from the pig. Then six human genes that would improve acceptance of the transplanted organ were introduced, while another gene that allows pig heart tissue to grow excessively was also removed.
In addition to this, the transplant also required approval from the U.S. Food and Drug Administration (USFDA), which was granted on an emergency basis on New Year's Eve on compassionate grounds. Bennet was found ineligible to join the transplant list while his arrhythmia made him unsuitable to receive an artificial heart pump as well. His only hope of staying alive was the heart-lung bypass machine and the first-of-its-kind transplant from a pig.
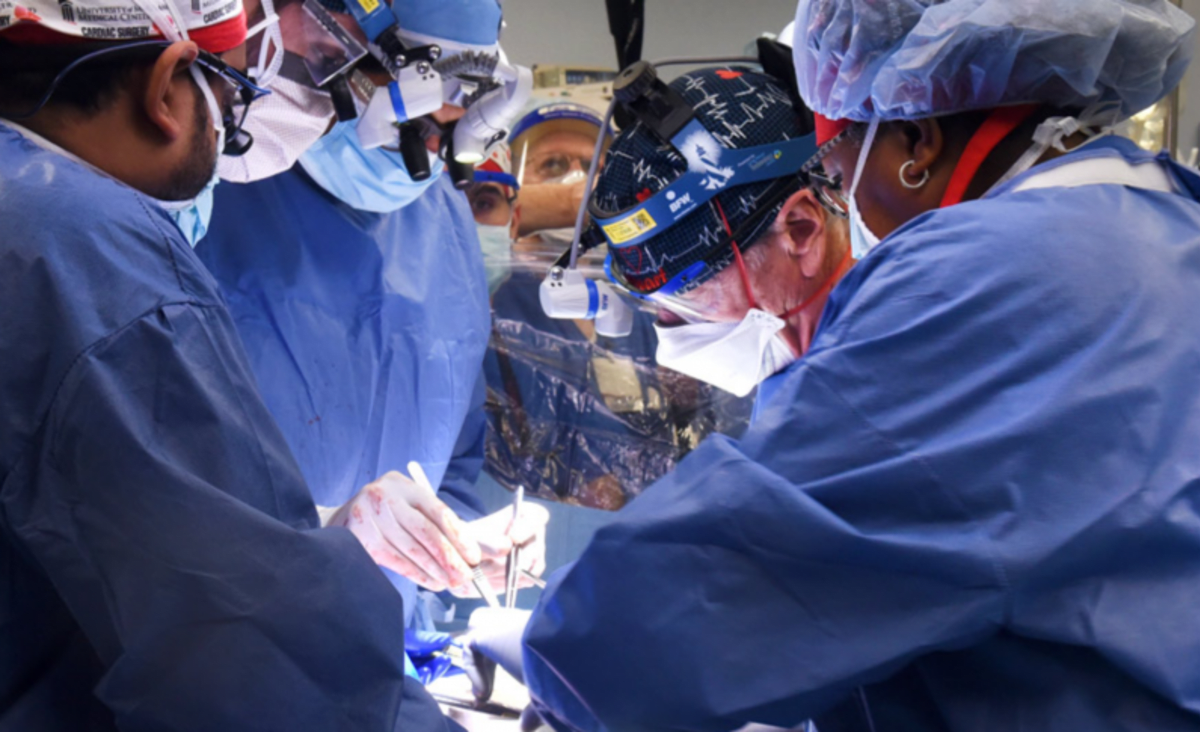
Prior to consenting to the transplant, Bennet was told about the risks of the procedure as well as its experimental nature. The surgical team at UMMC removed the heart from the donor pig and placed it in a device that preserved it until it was transplanted. To improve the chances of acceptance of the organ, the surgeons also used a new anti-rejection drug made by Kiniska Pharmaceuticals along with drugs that are conventionally used in transplant surgery, the press release added.
It is has been over three days that the surgery was performed and Bennet will now be monitored at the facility for a few weeks to evaluate the transplant's benefits. "This was a breakthrough surgery and brings us one step closer to solving the organ shortage crisis. There are simply not enough donor human hearts available to meet the long list of potential recipients," said Bartley P. Griffith, MD, who led the surgical team that carried out the transplant. "We are proceeding cautiously, but we are also optimistic that this first-in-the-world surgery will provide an important new option for patients in the future."
In July last year, an artificial heart was also transplanted into a human for the first time in the U.S.